Health experts like to warn that “disease knows no borders.”
It was true for El Paso and Juárez at the U.S.-Mexico border, two cities a river’s width apart. COVID-19 ripped through families on both sides as if the border didn’t exist, changing and ending lives regardless of nationality.
The two cities confronted waves of COVID-19 that hit within days or weeks of each other. The virus took a terrible toll on the lives of Borderland residents, overwhelming hospitals, shuttering businesses and isolating previously intertwined communities.
More than 3,300 people have died in El Paso; more than 4,500 have perished in Juárez.
Texas border counties were some of the hardest-hit in the state. U.S. border crossings were closed to most Mexican nationals for nearly two years, separating binational families and communities. Both cities suffered parallel economic losses.
Among the top lessons learned from the past two years is that the U.S. and Mexico, El Paso and Juárez, need to work more closely together on pandemic crisis management, according to research and interviews with more two dozen experts in border health. The El Paso Times and Puente Collaborative examined what worked in the global fight to contain the pandemic and future strategies to cope with disease threats at the border.

Mark Lambie/El Paso Times
El Paso and Juárez officials opened lines of communication and tried to find ways to share resources, like vaccines. But divisive politics and a lack of federal support, from either Washington D.C. or Mexico City, hindered deeper collaboration that could have saved lives.
“At a time when we were very polarized about borders in particular, this disease comes along that forces both the northern border of Mexico and the southern border of the United States to be isolated, politically and geographically,” said Dr. Manuel de laRosa, vice president for community engagement at Texas Tech University Health Sciences Center and a member of the U.S.-Mexico Border Health Commission.
Binational plans laid by the U.S. and Mexico in the wake of past, less lethal pandemics were largely ignored and vehicles for addressing Borderland health had been weakened.
When COVID-19 hit, the North American Plan for Animal and Pandemic Influenza — a guide to cooperatively addressing disease threats for the U.S., Mexico and Canada — wasn’t broadly put into action, analysts say. The North American Leaders Summit, where issues of cross-border health were once discussed, hadn’t been held since 2016. The U.S.-Mexico Border Health Commission, tasked with improving well-being in the Borderland, had seen its funding decline and activities curbed.
BRIANA SANCHEZ/EL PASO TIMES
“Border cooperation is difficult,” said Julie Collins-Dogrul, associate professor of sociology at Whittier College who studies border health. “That means we need everything we can do at multiple levels to help facilitate that communication, to legitimize it and to say it’s important.”
Health authorities say after two years of experimentation in pandemic crisis management, border communities have a lot to learn from one other. At great odds, sister cities from Texas to California found creative ways to share resources and coordinate responses.
It was too expensive and too many people died for us to walk away from it.
San Diego vaccinated Tijuana maquila workers, and El Paso did the same for factory workers in Juárez. New Mexico’s health department shared contact-tracing information with counterparts in Chihuahua state. A Douglas, Ariz., health clinic closely coordinated disease surveillance with nearby hospitals in Agua Prieta, Sonora.
El Paso County Judge Ricardo Samaniego said binational communities need to come together to learn from one another — however painful reliving any part of the past two years may be.
“It was too expensive and too many people died for us to walk away from it,” Samaniego said.
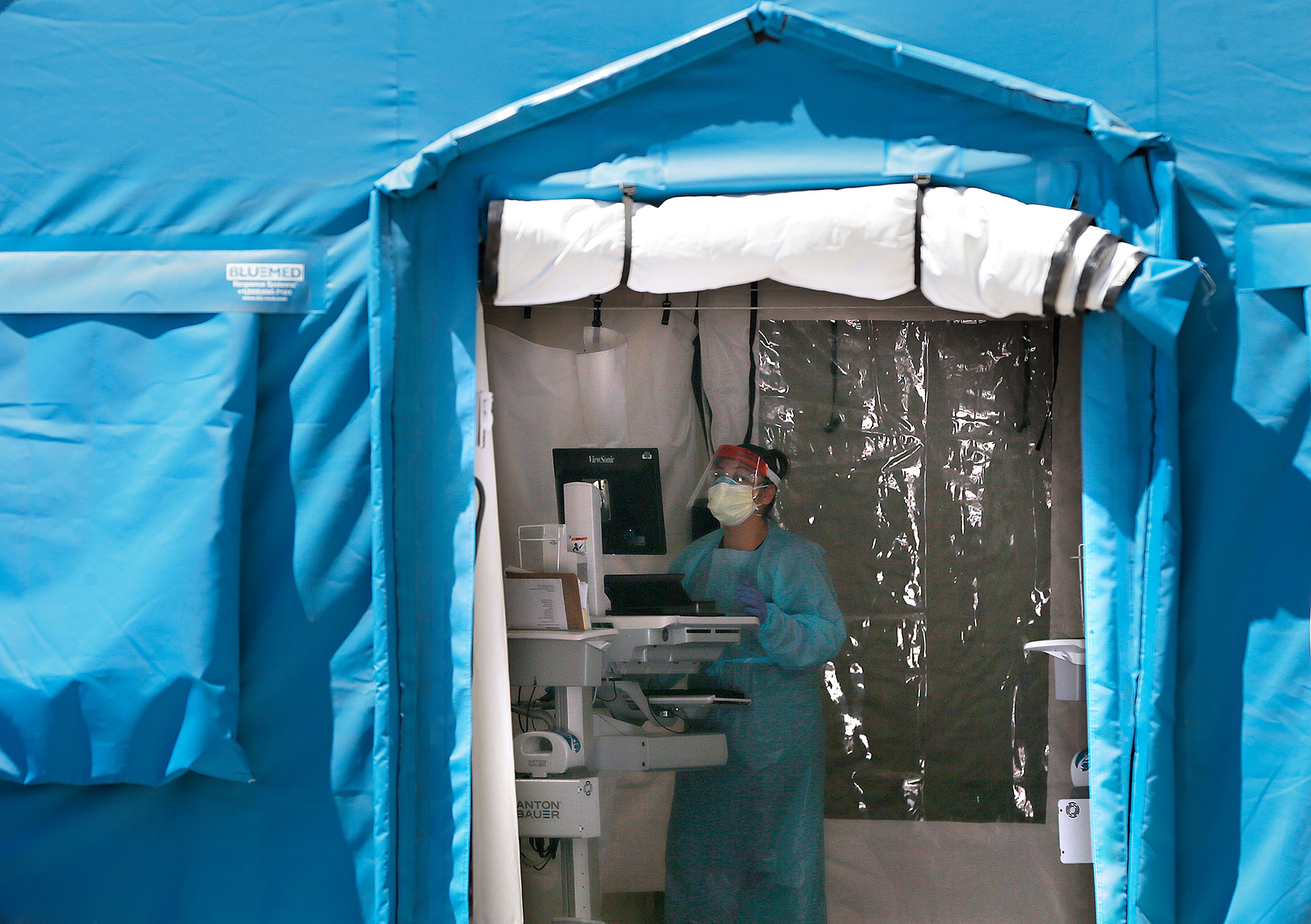
Mark Lambie/El Paso Times
There were many unknowns at the beginning of the pandemic: doubts about how the novel coronavirus spread, what policies would be most effective at curbing transmission, who was at greatest peril.
“Our first case was detected that night on March 13,” said Dee Margo, who was the El Paso mayor in 2020. “We started gearing up to deal with an unknown, and we didn’t know the severity.”
The United States had inordinately more resources to fight the pandemic than Mexico. Government spending on health care in Mexico was a mere $607 per capita in 2020, according to the Organization for Economic Cooperation and Development. The United States spent $9,054 per capita in 2019, according to the most recent data available.
In the Borderland, officials in two countries with vastly different resources and health systems confronted the same threat.
People living near the U.S.-Mexico border faced enormous risks. El Paso and Juárez share high rates of diabetes, obesity and hypertension — conditions that made COVID-19 more lethal. Multi-generational households, a norm in the Borderland, meant vulnerable seniors could be more exposed to the virus.
BRIANA SANCHEZ/EL PASO TIMES, BRIANA SANCHEZ
In the U.S., federal spending cuts had hobbled border health offices charged with coordinating with Mexico on health issues.
“Instead of having one resource to ride into that effort, we basically had to say, New Mexico what can you do? El Paso what can you do?” Travis Leyva of the New Mexico Office of Border Health in Las Cruces said. “We were limited.”
The Centers for Disease Control and Prevention declined an interview request.
COVID-19 binational health to prepare for more pandemics
The COVID-19 pandemic hit the Borderland hard.
More than 7,800 people have died in El Paso and Juárez.
Anthony Jackson, El Paso Times
As local leaders scrambled, the U.S. and Mexican governments turned inward. The U.S. prohibited non-essential travel at land border crossings beginning on March 21, 2020, and although the effort was billed as a “joint” decision with Mexico, the Mexican government never restricted southbound travel.
Border restrictions were one of many political responses to the pandemic lacking a clear public health rationale — although hundreds of countries opted for border closures in response to COVID-19. A recent study of border restrictions worldwide found no correlation between the bans and a reduced spread of COVID-19. The World Health Organization has discouraged against border closures as a method of pandemic control.
Omar Ornelas/ El Paso Times
The U.S. Department of Homeland Security extended the “temporary” restrictions on non-essential travel month after month, for nearly two years. Still, because U.S. citizens and legal permanent residents were exempted, El Paso and Juárez saw an average of half a million or more crossings of personal vehicles at area international bridges in 2020; the number neared 800,000 before the restrictions were lifted in November 2021, according to the Border Regional Modeling Project at the University of Texas at El Paso.
The politicization of the crisis made it harder for health leaders to do their job effectively — especially where two countries, three states and two cities govern a population of 2.5 million people.
“You would think public health would not be embroiled in politics,” said Alicia Thompson, health director for Cochise County, Arizona, on the border with Sonora, Mexico. “But the way that public health is structured in the United States, there has always been a political component to the work that we do.”
The Mexican Consulate in El Paso held a meeting in the early days of the pandemic to bring together leaders from Juárez and El Paso, Chihuahua and Texas. The consuls general in both cities; Margo and then-Juárez Mayor Armando Cabada; El Paso County Judge Ricardo Samaniego and the cities’ respective health authorities, gathered around a table, with the chairs set at some distance.
Information was shared. Pledges were made to collaborate.
“We made a show of caring about each other,” said Juan Acereto, a former Mexican consul who serves as liaison to the U.S. for the Juárez municipal government. “But in the end, we each retreated to our respective homes. We became selfish.”

Omar Ornelas/El Paso Times
Health authorities in El Paso and Juárez did stay in frequent contact, according to El Paso health and emergency management authorities. But much of the communication was informal, people calling each other up to share information and plans. “You had this tremendous disconnect between our recommendations and advice and what we’re doing versus what they’re doing,” Margo said.
El Paso’s epidemiologist held daily calls with the epidemiologist responsible for Juárez, said El Paso Fire Chief Mario D’Agostino.
“I had a personal communication with the Juárez health authority,” said Dr. Hector Ocaranza, El Paso County’s health authority. “That was done via phone, as well. Having that informal communication, we shared plans, we shared also other new medical information, how we’re going to be responding to a particular situation that might be arising. That’s what we would do.”
Leyva in Las Cruces said in the early months his office would notify Chihuahua of binational cases — residents with ties to Chihuahua who tested positive in New Mexico — so they could contact-trace south of the border. But eventually the volume was too great.
“Once the cases were in the hundreds daily, it was very difficult to do that,” Leyva said. “Then we switched over from case investigation into community awareness.”

Aaron E. Martinez/El Paso Times
Case numbers and hospitalizations spiked in the Borderland region in October 2021.
COVID-19 waves tended to coincide in neighboring Las Cruces and El Paso. But according to an El Paso Matters/Kaiser Health News analysis, New Mexico border counties fared better than Texas border counties.
The analysis found from March 2020 to January 2021, residents of El Paso County under 65 died of COVID-19 at a rate 70% higher than those of neighboring Doña Ana County, New Mexico. Texas has a higher rate of uninsured residents than New Mexico, and restrictions like mandatory masking were more stringent in New Mexico than Texas.
The Texas Department of State Health Services, which runs the Office of Border Health, declined an interview request.
When the fall 2020 spike passed, and vaccines began to arrive in U.S. border counties, binational communities began to work together in new ways.
Five University Medical Center nurses were the first El Pasoans to be vaccinated on Dec. 15, 2020. A vaccination campaign in Juárez began four months later on April 12, 2021 — but vaccines trickled into northern Mexico slowly, with months-long gaps between available shots.
Omar Ornelas/ El Paso Times
As Mexicans waited, some supplies of vaccines in the U.S. neared their expiration date. The border remained closed to non-essential travel and only President Joe Biden could authorize the donation of vaccines to Mexico.
The U.S. made its first donation of 1.7 million shots to Mexico in June 2021, but U.S. border communities were clamoring for opportunities to share vaccines more quickly with sister cities. Ultimately, the U.S. would donate more than 14.1 million vaccines to Mexico.
Dr. Cecilia Rosales, chair of the Division of Public Health Practice & Translational Research at the University of Arizona in Phoenix, led an effort to establish vaccine clinics inside ports of entry for Mexican nationals — something El Paso leaders achieved for thousands of maquila and farm workers but couldn’t provide for other Juárez residents.
Arizona clinics vaccinated more than 33,000 Mexican nationals at ports of entry during the border restrictions.
BRIANA SANCHEZ/EL PASO TIMES
Health leaders across the border region in the U.S. and Mexico say they did the best they could with the information available at the time. But looking forward, many said they hope to formalize cross-border networks built over the past two years.
“I think what we’ve learned from this pandemic is the need for us to really standardize, especially these projects that we have with Mexico,” Rosales said.
Jimmy Kolker, a former assistant secretary for global affairs in U.S. Health and Human Services who oversaw the U.S.-Mexico Border Health Commission, testified in the Senate in June 2020 on the urgency of fighting the COVID-19 pandemic in tandem with Mexico. There was no time to wait, he said.
“If you think of this as a fire raging across an entire city… we have got to work with our neighbors to put the fire out,” he said. “Because there is nothing we can do to protect our home that will not require us also working with our neighbor.”
Martha Pskowski can be reached at mpskowski@elpasotimes.com
Lauren Villagran can be reached at lvillagran@elpasotimes.com
Visuals journalists Omar Ornelas, Anthony Jackson, Briana Sanchez, Aaron E. Martinez contributed to this report.




